Lyme Disease Is Not What Most Doctors Think It Is
The conventional understanding of Lyme disease — a tick-borne infection caused by Borrelia burgdorferi, producing a bull’s-eye rash and treatable with a few weeks of antibiotics — represents only a fraction of the clinical reality. Research that the Frequency Research Foundation has been tracking for over two decades paints a far more complex and consequential picture.
Lyme disease is now considered one of the fastest growing infectious diseases in the world. In the United States alone, estimates suggest at least 200,000 new cases per year, with some researchers believing that as many as one in fifteen Americans may be currently infected. The disease can mimic dozens of other conditions, it may spread through routes beyond tick bites, and it has been linked to neurodegenerative diseases including Alzheimer’s and Parkinson’s.
This article brings together key research findings that challenge the conventional narrative and explain why Lyme disease deserves far more attention — and far more sophisticated treatment — than it currently receives.
The Spirochete: A Uniquely Dangerous Organism
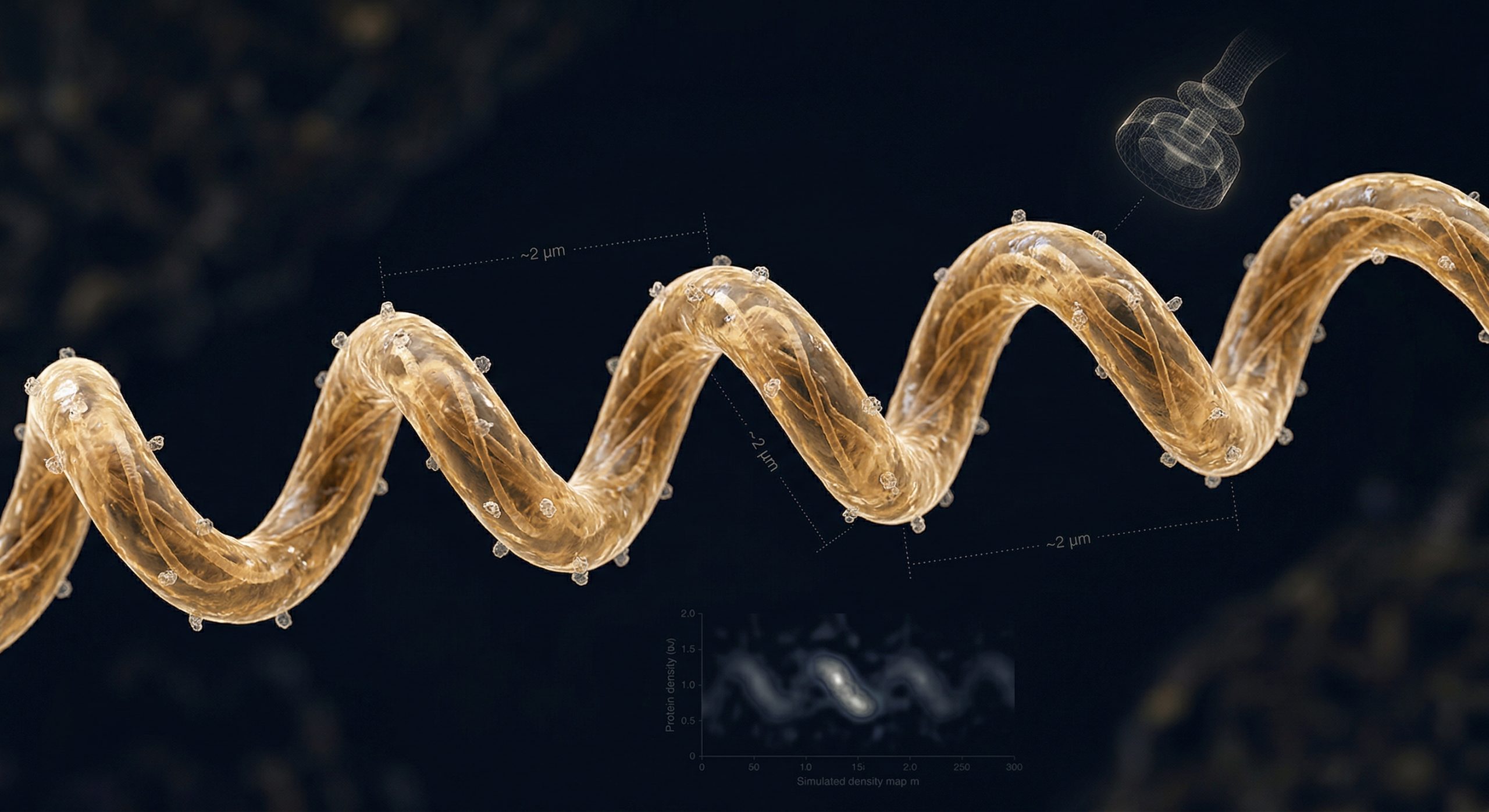
Borrelia burgdorferi, the spirochete responsible for Lyme disease, is not an ordinary bacterium. Its corkscrew shape allows it to burrow into tendons, muscle cells, ligaments, and directly into organs — including the brain. This invasive capability is what makes Lyme disease so devastating and so difficult to eradicate.
The Disease Mimicry Problem
One of the most significant challenges with Lyme disease is its ability to mimic other conditions. Research has documented Lyme presenting as or contributing to amyotrophic lateral sclerosis (ALS), Parkinson’s disease, multiple sclerosis, Bell’s palsy, reflex sympathetic dystrophy, neuritis, psychiatric illnesses including schizophrenia, chronic fatigue syndrome, heart failure, angina, irregular heart rhythms, fibromyalgia, dermatitis, autoimmune diseases such as scleroderma and lupus, eye inflammatory reactions, sudden deafness, ADD and hyperactivity, and chronic pain syndromes.
This extraordinary range of presentations means that many people carrying active Lyme infections are being treated for other diagnoses — receiving medications that address symptoms but not the underlying infectious cause. The implications for healthcare costs and patient outcomes are enormous.
Cell Wall Deficiency: The Stealth Factor
Dr. Lida Mattman, biology professor and author of Cell Wall Deficient Forms: Stealth Pathogens, demonstrated a critical characteristic of Borrelia burgdorferi that explains much of its treatment resistance. The spirochete can survive and spread in a cell wall deficient (CWD) form — essentially shedding its cell wall to evade both the immune system and antibiotics.
Many of the most valuable antibiotics work by targeting bacterial cell walls. When Borrelia shifts to its cell wall deficient form, these antibiotics become ineffective. The organism persists in the body despite treatment, capable of reverting to its active spirochete form when conditions are favorable.
This parallels what we observe with mycoplasma — another cell wall deficient organism that plays a central role in chronic Lyme disease. Our articles Mycoplasma: A Key Component in Lyme and Other Diseases and Mycoplasma – Why the Lyme Flu Goes On and On cover this critical co-infection in detail.
Transmission: Beyond the Tick Bite
One of the most significant and controversial findings in Lyme research involves potential routes of transmission beyond the standard tick bite narrative.
Evidence for Broader Transmission
Dr. Mattman’s research demonstrated the recovery of live Borrelia spirochetes from mosquitoes, fleas, mites, semen, urine, blood, and spinal fluid. This suggests that the organism is present in multiple body fluids and potentially transmissible through routes that conventional Lyme guidance does not acknowledge.
Dr. Robert Rowen documented a family in which a mother’s Lyme infection appeared to spread to five of her six children, all of whom recovered with appropriate therapy. As Dr. Howenstine noted in his analysis, it is difficult to believe that all of these children were bitten by infected ticks — person-to-person transmission within the family is a more plausible explanation.
Dr. Mattman stated directly: “I’m convinced Lyme disease is transmissible from person to person.”
These findings, while debated within the medical community, have significant implications. If Lyme can spread through routes beyond tick bites, the actual number of infected individuals may be far higher than official estimates — and the approaches to prevention and screening need to be fundamentally reconsidered.
Lyme and Neurodegenerative Disease: The Critical Connection
Perhaps the most alarming finding in Lyme research is the connection to neurodegenerative disease. This is directly relevant to the Frequency Research Foundation’s work on Alzheimer’s disease.
Dr. Mattman’s Findings
Dr. Mattman’s laboratory work produced extraordinary results when testing patients with neurodegenerative conditions for Borrelia. She recovered Borrelia spirochetes from 8 out of 8 cases of Parkinson’s disease tested, from 41 cases of multiple sclerosis, from 21 cases of amyotrophic lateral sclerosis, and from all tested cases of Alzheimer’s disease.
In 1995, Dr. Mattman obtained positive cultures for Borrelia from 43 of 47 persons with chronic illness — a 91% positivity rate — while only 1 of 23 healthy control patients tested positive.
These findings suggest that Borrelia burgdorferi may be far more prevalent in neurodegenerative disease than conventional medicine recognizes. If confirmed at scale, the implications are staggering: a significant proportion of cases diagnosed as Parkinson’s, MS, ALS, and Alzheimer’s may have an underlying infectious component that is being completely missed — and that is potentially treatable.
Recovery From “Terminal” Conditions
Dr. Howenstine reported that several patients with terminal amyotrophic lateral sclerosis achieved complete recovery after receiving appropriate Lyme disease treatment. This finding, while based on small numbers, underscores the critical importance of testing for Borrelia in patients with neurodegenerative diagnoses.
If even a fraction of neurodegenerative disease cases involve treatable Borrelia infections, the failure to test for Lyme in these patients represents a significant clinical oversight.
The Broader Infectious Theory of Alzheimer’s
Dr. Mattman’s findings regarding Borrelia in Alzheimer’s patients align with a growing body of evidence implicating chronic infections in Alzheimer’s disease. As documented in our article Alzheimer’s and Herpes Simplex Virus, herpes simplex virus type 1 DNA has been found in 90% of Alzheimer’s plaques. Mycoplasma and other chronic infections add additional layers of neuroinflammatory burden.
The emerging picture is that Alzheimer’s disease may, in many cases, be driven by a combination of chronic infections — viral, bacterial, and mycoplasmal — that sustain the neuroinflammation and amyloid accumulation characteristic of the disease. Our complete guide to Alzheimer’s disease and frequency therapy covers this multi-pathogen theory and the frequency-based approaches designed to address it.
2026 Update: What Has Changed Since This Article Was Published
Lyme disease research has advanced significantly, and several of the findings discussed in this article have been reinforced or expanded by subsequent work.
Chronic Lyme Is Now More Widely Acknowledged
The existence of persistent Lyme disease symptoms after standard treatment — long denied by much of the medical establishment — is now more widely acknowledged. The term “Post-Treatment Lyme Disease Syndrome” (PTLDS) is used in mainstream literature, though the Frequency Research Foundation’s position remains that ongoing symptoms typically reflect ongoing infection (including co-infections like mycoplasma) rather than a mysterious post-infectious syndrome.
Borrelia Persistence Confirmed
Multiple studies have now confirmed that Borrelia can persist in the body despite antibiotic treatment. Research published in journals including PLOS ONE and the Journal of Clinical Microbiology has demonstrated the survival of Borrelia in various tissue types after antibiotic courses — confirming what Dr. Mattman documented decades earlier with her cell wall deficient forms.
The Lyme-Alzheimer’s Connection Gains Support
The broader infectious theory of Alzheimer’s disease — which encompasses Borrelia alongside HSV-1, mycoplasma, and other pathogens — has gained substantial mainstream support since this article was published. Major research institutions now investigate the role of chronic infections in neurodegeneration, and the concept that amyloid beta functions as an antimicrobial peptide (produced by the brain in response to pathogens) provides a mechanistic framework that accommodates Dr. Mattman’s finding of Borrelia in Alzheimer’s brains.
Lyme Disease Prevalence Continues to Rise
CDC estimates of Lyme disease incidence have been revised upward repeatedly. The agency now acknowledges approximately 476,000 new cases per year in the United States — more than double the earlier estimates cited in the original research. Geographic spread has expanded significantly, with Lyme now reported in all 50 states.
Frequency Protocols Have Advanced
The Frequency Research Foundation’s Lyme disease protocols have been refined continuously. Our latest version, Lyme Frequencies Version 11.0, represents over two decades of development and addresses the full Lyme complex — spirochetes, mycoplasma co-infections, viruses, fungi, and nanobacteria — in a systematic, sequential approach.
Why Frequency Therapy for Lyme Disease
The characteristics that make Lyme disease so difficult to treat with conventional antibiotics — cell wall deficiency, tissue burrowing, intracellular persistence, co-infections — are precisely the characteristics that frequency therapy is designed to address.
Addressing the Full Complex
Standard antibiotic treatment targets Borrelia spirochetes in their active, cell-walled form. It does not address cell wall deficient forms, mycoplasma co-infections, viral co-infections, or fungal co-infections. As Dr. Jeff Sutherland has observed in clinical practice, the spirochetes can be addressed relatively quickly with frequencies, but the complete resolution of Lyme disease requires systematically addressing every organism in the complex.
Reaching Hidden Organisms
Borrelia burgdorferi burrows into tissues, hides inside cells, and converts to cell wall deficient forms that evade standard treatment. Frequencies are not limited by these defense mechanisms — they can reach organisms regardless of their location or form.
Managing Complex Co-Infections
The Lyme disease complex typically involves multiple organisms that interact synergistically. Frequency therapy allows multiple pathogens to be addressed within the same treatment framework, with careful sequencing to manage Herxheimer reactions as organisms are eliminated.
Our article [Cause, Spread, and Therapy of Lyme Disease](INSERT CAUSE SPREAD URL) provides a comprehensive overview of the Lyme disease treatment approach, while the mycoplasma component is covered in detail in our dedicated mycoplasma articles.
Dealing with chronic Lyme, unexplained neurological symptoms, or a neurodegenerative diagnosis? The research suggests that infectious causes — particularly Borrelia and its co-infections — may be a contributing factor. Dr. Jeff Sutherland offers personalized paid consultations to assess your situation and develop a comprehensive frequency protocol. Book Your Consultation
Frequently Asked Questions
Take the Next Step
The research on Lyme disease reveals a picture far more complex and far-reaching than most patients or physicians realize. If you are dealing with chronic Lyme, persistent symptoms after treatment, or a neurodegenerative condition that has not responded to conventional approaches, the infectious component may not have been fully addressed.
Dr. Jeff Sutherland has spent over two decades developing and refining frequency protocols for the complete Lyme disease complex. A paid consultation can assess your specific situation and develop a targeted treatment plan.
Book Your Consultation with Dr. Jeff Sutherland
This article is part of our comprehensive Alzheimer’s resource library. Lyme disease and its co-infections are now recognized as potential contributors to Alzheimer’s and other neurodegenerative conditions. Read our complete guide to Alzheimer’s disease and frequency therapy for the full scope of research on infections, environmental toxins, nutritional strategies, and frequency-based treatment approaches.
© Frequency Research Foundation. This content is for educational and informational purposes only. It is not intended to diagnose, treat, cure, or prevent any disease. Always consult with qualified healthcare professionals regarding medical conditions.